We introduce a special report by two specialists in children and young people’s mental health on a pioneering school qualification.
“Children and young people’s mental health and wellbeing is a priority for the Scottish Government. It is central to achieving its ambition for Scotland to be the best place in the world for children to grow up,” Is how Audit Scotland puts it.
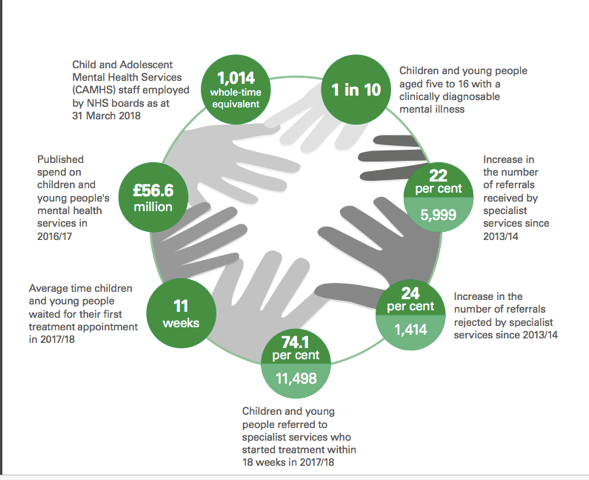
Yet, as is often the case in modern Scotland, good intentions about early intervention and prevention are not enough: the reality is a 30% leap (+8400) in referrals to specialist care services (CAMHS or Children & Adolescents Mental Health Services) in just five years to 2018, a jump in rejected referrals and a trebling in numbers waiting more than a year for starting treatment when the target is for 90% to get an initial appointment within 18 weeks. A fifth of young adults reported possible psychiatric disorders in 2016. Self-harming, especially among girls and young women, is endemic. And, the saddest statistic of all, 64 15-24 year-olds took their lives in 2017.
Poverty is at the root of this human crisis. Already, one in five Scottish children live in relative poverty with the incidence set to rise to 38% by 2030. But poverty, according to NHS Scotland, is just one of the stressful experiences that inflict mental health problems on young people and children – along with “abuse and neglect” and “family conflict, poor parenting, childhood adversity (ACEs), unemployment, chronic health problems and poor housing.” Life as trauma.
But this unresolved social catastrophe is exacerbated by a service that is unfit for purpose: a system that Audit Scotland describes as “complex and fragmented” and a service that appears seriously under-funded, with just 6% of NHS mental health spending devoted to our children and young people although this has risen in real terms 12% in five years. The Scottish Government has committed to spending a further £250m over the next five years. But this is a pin-prick.
There is no separate government strategy for children and young people’s mental health yet professionals, experts and commentators all agree we need a step change in approach and praxis. “Transforming services will only be possible with a clearer view of what works, a plan for how the system needs to change and a move away from reliance on short-term and isolated initiatives,” says Audit Scotland.
Meanwhile, as our twin authors report below, Scotland has developed the world’s first qualification award for mental health and well-being. “The basic premise is that understanding mental health should be a core skill to help us all manage mental health, increase resilience and reduce stigma. We would further argue that this should be as core to school learning as the 3Rs,” Anne McKechnie tells us.
“An investment in knowledge pays the best interest” Benjamin Franklin
Learning about mental health and wellbeing
How it all began… in Anne’s words
Recent years have seen a rise in concerns about the mental health of our young people. Charities, third sector and statutory bodies all share an anxiety that rates of poor mental health are increasing in children and adolescents, with accompanying cries of despair at long waiting lists and inadequate responses from CAMHS.
The Good Shepherd Centre is based in the West of Scotland (Renfrewshire) and accommodates up to 28 young people aged between 12 and 18, with 18 of those places for young people who are in need of secure care. They are referred under the Children’s Hearing System, or the Courts owing to concerns about risk to their own or others’ safety. In 2011, as an independent consultant forensic clinical psychologist, I was asked to set up a service, going in once a week to assess and treat young people, as well as consulting to and supporting staff.
The young people in that setting have, without fail, been exposed to trauma and adversity. More often than not, they have also been referred to children and adolescent services for assessment in the context of concerning behaviours such as self-harm, running away, overdosing, violence or substance misuse. Given the huge stigma about mental illness, and often resentment at potential interpretation of risky behaviours as evidence of madness, unsurprisingly the young people are often reluctant to be seen by yet another mental health professional. Add to that the shame and self-blame that often accompanies childhood neglect or trauma, subsequently refusal or recalcitrance are not unusual.
Psycho-education
When treating any mental illness, psycho-education has widely been recognised as the first step toward improved coping. Offering someone in distress the opportunity to understand objectively what is happening to their mind effectively removes stigma and shame, thereby opening up the opportunity to learn how to manage the anguish associated with anxiety, low mood – even aggression. Such therapeutic intervention is most often offered in the context of psychological therapy and therefore by mental health professionals.
Given the anxiety, mistrust and certainty that all thoughts are transparent to a psychologist, many of the young people in the Good Shepherd were reluctant to engage in this first step toward improved coping. They were anxious about how this would be viewed by their peers as well as sometimes fearful of appearing stupid or “really mad”. It was with this insight that I approached the education department at the Good Shepherd.
All young people in secure care are expected, encouraged and supported to engage in some form of education. The school day is highly structured with small classes offering a range of topics within the wider curriculum but also designed to appeal to minds mistrustful of authority and sensitive to criticism and failure. What better environment to learn how our brains and emotions work? We have all learned about how to keep ourselves physically healthy, why should mental health be any different?
Education staff were all hugely enthusiastic about the proposal to create a special qualification in mental health, recognising that if young people could learn about their brains, how to recognise and regulate emotions, how to cope more effectively and thereby reduce stress and lift mood, learning would be a natural consequence. The Scottish Qualifications Authority, on hearing of this initiative, offered to host a Qualifications Development Team and thus was born the world’s first ever school qualification in Mental Health and Wellbeing. The work progressed incredibly quickly with input from mental health, education and social care; aims and content were, notably, shared and agreed by all – a reflection of a shared sense of the importance and timeliness of such a development.
The roll out of the award….
Shelley Buckley writes:
In January 2019 I left my post as teacher in the Good Shepherd Centre to work as a writer and subject implementation manager for SQA. I didn’t begin my career as a teacher but was led there through my experiences as a social worker in mental health services. It became clear to me, as a social worker, that what was lacking was a psychosocial model for mental health, which supported prevention and early intervention.
Even within crisis services, the dominance of the medical diagnosis and treatment limited the ability to work with the lived experience of the patient and support meaning making. The medical approach assumes a biological and physiological reason for illness which can therefore only be treated by a specialist using medical approaches.
Mental health as a subject is extremely contested and there are many schools of thought in relation to diagnosis and treatment. What even the most expert in the field can agree on is: it is not an exact science; the complexity of our mental wellbeing and how to maintain, much less treat, our mental health is an enigma and an area for which we as a society increasingly seek professional and specialist support.
Being mentally healthy
By taking a broader and longer view of public health and social policy, it became apparent to me that the embedding of psychosocial education in mental health within schools not only seemed the most pragmatic approach, but also supported the need for beginning a societal conversation about what it means to be mentally healthy. I have been working with schools and colleges across Scotland – both promoting the rationale for having psycho-education embedded within school curricula but also recognising that overwhelmingly teachers are themselves experiencing pressure from high workloads and performance-related processes which give greater priority to attainment than student experiences and meaning making.
However, despite this, the enthusiasm for the award is palpable and visible, demonstrated by the effort being made to consider creative ways to include it in an already packed curriculum. Teachers have frequently commented on the dire need for such education not just for young people but also for teachers and parents. Many of the discussions have raised questions around the skills and knowledge required to support and facilitate discussions, and there is a genuine fear around talking about associated subjects that are frequently associated with stigma.
Currently, teacher training does not have mental health education as part of core training and there is no recommended pathway for professional development in relation to mental health education, even for pastoral care teachers. Many teachers have highlighted concern around potentially difficult subject areas and language: “Can we use the term ‘mental illness’”; “Is it appropriate to discuss self-harm, family relationships and sexuality?” “What if we open up a can of worms?”
Making sense of it all
This award allows for discussion of these issues; for how do we make meaning unless we truly understand the way in which we perceive the world and language we use to relate to one another, the context of our lives and the choices we make. Language is everything, especially when we are discussing mental health; it has the power to profoundly change the course of someone’s life, especially when we get into the realms of potential medical diagnosis and intervention. The universality of schools and colleges means that a level of knowledge is accessible to all.
This is a subject that clearly does need to be unpacked. I have been fortunate enough to have been able to be involved in the start of conversations around what we really mean when we talk about mental health and being mentally healthy. It is also important that these conversations are informed, critical and part of a dynamic reflective education system. The course itself is designed as an open portfolio allowing the content to be developed and changed in accordance with evolving knowledge and the needs of the learner. It also allows for creative design around learning as well as learner involvement in the process of demonstrating understanding.
Outlook

Over the coming months we will both be working with colleagues at the Good Shepherd Centre. We will be using the award to support scaffolding to take young people through the process of understanding their mental health experiences. By providing a truly holistic approach to wellbeing, all Good Shepherd staff will work with the young people in building a range of coping strategies, resilience and self-care, that will have meaning and relevance in the lives of the young people and their destinations post Good Shepherd Centre.
Images via Good Shepherd Centre and Audit Scotland
Further reading:
Scottish Children’s Services Coalition calls for investment, Common Space, July 5 2019
Stressed teachers, The Herald, July 5 2019
Children left for months, STV News, June 5 2019


Leave a Reply